
One of the most important factors determining the accuracy and reliability of laboratory tests is you. Proper preparation is essential, to ensure the quality of your test results! Below, please find information you need to know prior to your tests.
The definition of fasting (abstinence from food) refers to a state of not eating food or drinking liquids for a period of about 12 hours. Only non-carbonated (still) water should be drunk before blood is drawn for the laboratory tests.
It is recommended to avoid drinking coffee and tea, or consuming chewing gum. Certain substances can interfere with the glucose test results. Caffeine increases your blood sugar levels.
Prolonged fasting (>12 hours) before blood draws is not recommended, especially in patients with low body fat. This can lead to too low blood sugar levels, and even an increase in ketone bodies, as well as low iron and haemoglobin levels.
| Iron level test | Do not use iron supplement for 1–2 days |
| Vitamin D | Do not take vitamin D supplements in therapeutic doses for 24 hours. |
| Thyroid function tests | Do not take l-thyroxine or other thyroid medication on the day before the blood test. |
| vitB12 Vitamin B12 | Do not take the supplement for 2–3 days. If you had an IV drip for supplements (B12 and B9) after IV drip please wait 1–2 weeks before conducting a blood test for vitamins B9 and B12. |
| FA Folic acid (vitamin B9) | Do not take biotin supplements for at least 48 hours. |
| Active vitamin B12 | Do not take the B12 supplement for 2–3 days. Do not take biotin supplements for at least 48 hours. |
| .Vitamin C (ascorbic acid) | Do not take the Vitamin C supplement for 2–3 days. |
| Vitamin H (biotin) | Do not take the investigational vitamin supplement for 2–3 days. |
| Vitamin K (Phylloquinone) | Do not take the investigational vitamin supplement for 2–3 days. |
| Vitamin B1 (thiamine) | Do not take the investigational vitamin supplement for 2–3 days. |
Interference of biotin with the laboratory test results
As biotin interferes with many laboratory tests, the patient should discontinue the consumption of biotin (multivitamins or supplements containing biotin or "Vitamin B7") for 48 hours or more before the laboratory test, to minimise interference with the test.
Biotin interferes with the following tests:
| Active vitamin B12 (AB12) | Cytomegalovirus IgG antibodies (CMV) | Free beta human chorionic gonadotropin (B-HCG) | N-terminal B-type (brain) natriuretic pro-peptide (NT-proBNP) | Thyroglobulin (Tg) |
| Cyclic citrullinated peptide antibodies (anti-CCP) |
Cytomegalovirus IgM antibodies (CMV) | Free thyroxine (FT4) | Pregnancy associated plasma protein-A (PAPP-A) | Testosterone (TSTO) |
| Hepatitis B surface antigen antibodies (aHBs) | Estradiol (E2) | Hepatitis B core antigen antibodies (aHBcore) | Parathyroid hormone (PTH) | Combination HIV |
| Hepatitis C virus antibodies (aHCV) | Folic acid (FOL) | Hepatitis B surface antigen (HBsAg) | SARS-CoV-2 IgG antibodies | |
| Adrenocorticotropic hormone (ACTH) | Free prostate-specific antigen (fPSA) | Homocysteine (HCY) | Sex hormone binding globulin (SHBG) |
2-point glucose tolerance test (GTT) for pregnant women:
There are also certain requirements that need to be met before a glucose tolerance test:
If you plan to collect a urine sample for laboratory tests, we recommend using a disposable urine container. The urine is collected in a special disposable container, which is available at the pharmacy. The disposable urine container does not need to be washed or otherwise prepared. For babies and young children, a urine sample can be collected using urine collection bags.
NOTE: Please note that for microbiological tests (urine culture), the container must be sterile and kept in a sealed container.
NOTE: It is unacceptable to urinate in bottles, jars and other containers not intended for this purpose. Various substances such as sugar residues or bacteria can interfere with the test results.
For a few days (at least 10-12 hours) before the collection of urine for testing, we recommend following a standard diet and eating as usual, but avoid spicy, salty foods and products that can change the colour of the urine (e.g. carrots, beetroot, etc.), and to drink a normal intake of liquids with no alcohol. Avoid heavy physical activity and prolonged standing for longer than usual before the urine collection. Excessive exercise can lead to protein and ketone bodies in the urine, or an increase in their levels. Orthostatic proteinuria often occurs as a result of prolonged standing.
We recommend avoiding sexual intercourse for 24 hours before the urine sample collection. Urine testing after sexual intercourse can be complicated by the presence of semen in the urine. A high sperm count does not allow for a proper microscopic evaluation of the urine sediment. There may also be minor lesions in the urethra, which may result in the presence or an increase of epithelium and erythrocytes, or the detection of bacteria in the urine.
Avoid having a urine test during menstrual bleeding and for 2-3 days before and after menstruation. If necessary, these circumstances should be documented. When collecting urine samples during menstruation, the urine is often contaminated with erythrocytes and epithelium, making it impossible to obtain reliable results. Your doctor may interpret this result as haematuria.
Discontinuation of medicines is not necessary, but you should inform the laboratory and doctors of any medicines or food supplements you were taking at the time of the urine collection. Some of these substances may interfere with the results of urine tests:
Before collecting urine for the microalbumin/creatinine test, we recommend not taking the following medicines for 8–12 hours:
Before collecting the urine, it is necessary to find out the purpose and the method that is to be used:
| Purpose | Procedure |
|---|---|
| Morning urine | It should be collected after waking up, i.e. after a night's rest of 8 hours or, if this is not possible, at least 4 hours after the previous urination. |
| "Midstream portion" of the urine sample |
Neither the first nor the last portion of urine is collected; instead, the midstream portion sample is collected (20–50 ml). |
| "All day urine" | The urine is collected all day. When you get up in the morning, pee in the toilet and record the time. Then, all the urine is collected for a period of 24 hours. The last urine must be collected the next day, at the same time as on the first day. |
| STD urine test by PCR | Do not urinate for 3-4 hours before the collection, and do not wash the external genitals. The first portion of the urine is collected (“first drops”). |
| Urine for a cytopathology test | Collect the second portion of the day, 3-4 hours after the morning urination. |
A urine test is a quick and easy way to assess your kidneys and other organs, and to test for heavy metal poisoning, sexually transmitted diseases and other health problems. Statistics show that as many as 30% of people have changes in their urine, but these figures can also be distorted by the improper preparation for urine tests.
IMPORTANT: The urine for testing must be collected only in a disposable plastic container. Urine collected in other containers (jars, food containers, etc.) is not suitable for testing and will not be accepted. We do not recommend conducting a urine test with women during menstruation.
IMPORTANT: Different methods are used for urine tests (general clinical tests, molecular diagnostics (PCR) and microbiological tests), and they require different preparations (such as the first urine stream or midstream urine portion)! Here is the information you need to know, in order to prepare properly for your urine testing.
When you prepare for the collection of urine for testing, you must adhere to the following general rules:
.png)
You will need a disposable container for general and PCR tests, or a sterile container in a sealed package for microbiological tests.
The first portion of the urine is needed to detect sexually transmitted pathogens. The urine is tested by the molecular diagnostic (PCR) method using morning urine, or the patient must not have urinated for at least 4 hours.
Process of collecting the first portion of urine for men and women:
24-hour urine collection:
Process of collecting the midstream portion of urine for men and women:
For men

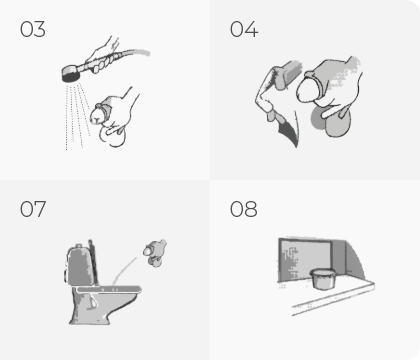
For women
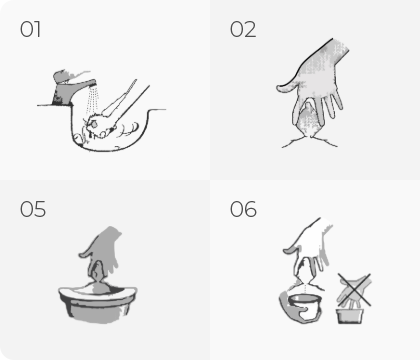
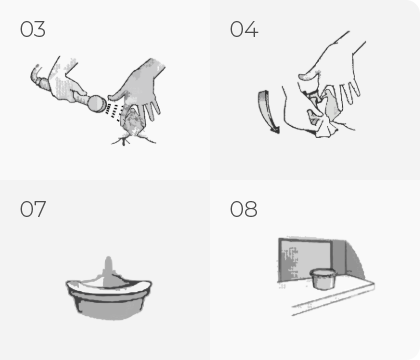
If you are planning to collect a stool sample for laboratory tests, we recommend using a plastic container. The stool shall be collected in a special disposable container, which is available at the pharmacy. You must also prepare a clean, dry container to collect the stool in. The coprological test is carried out without any special preparation on the part of the patient, who should be following a normal diet and not fasting or overeating. For people with constipation, stool collection can be a problem. To facilitate bowel movements, it is a good idea to increase the amount of fluid and fibre in your diet; for example, by including wholemeal cereals, bran, fruit and vegetables.
In the case of testing for human pinworms, the sample shall be taken by a general practice nurse.
Stool testing and medicines:
If you are taking other medicines, check with your doctor before taking the stool test to make sure they will not interfere with the results.
How to prepare for genital scraping:
Recommendations for women before genital scraping:
Recommendations for men: do not urinate for 2-3 hours before the collection of the genital scraping.
For two days before the PAP, the following is recommended:
Do not schedule a PAP smear during your menstrual cycle and for 4 days after. The best time to have a PAP test is at least 5 days after the end of your period, on Days 10-20 of your menstruation cycle.
In all cases, the test material (samples/ specimens) delivered to the laboratory shall be evaluated against the established criteria for its suitability for testing. If it does not meet the requirements, no tests shall be carried out. The reason shall be indicated in the order – MAC (Material Rejection Criterion). You will be informed of the established MAC, in accordance with the contractual procedure or in the test report.